Volume: 14 Issue: 1
Hematological Markers as Predictors of COVID-19 Severity: A Prospective Study from South India
Year: 2026, Page: 37-39, Doi: https://doi.org/10.47799/pimr.1401.25.69
Received: Oct. 7, 2025 Accepted: Dec. 25, 2025 Published: May 1, 2026
Abstract
Introduction: Coronavirus disease 2019 (COVID-19) demonstrates wide clinical heterogeneity, ranging from mild illness to severe pneumonia, acute respiratory distress syndrome, and multiorgan failure. Early identification of patients at risk of severe disease is essential, particularly in resource-limited settings. Simple hematological and inflammatory markers may aid in early prediction of disease severity. Methods: A prospective observational study was conducted on 100 RT-PCR–confirmed COVID-19 patients admitted between December 2020 and October 2022 at Prathima Institute of Medical Sciences, South India. Patients were categorized as critical or non-critical according to World Health Organization (WHO) severity criteria. Hematological indices and inflammatory markers, including neutrophil-to-lymphocyte ratio (NLR), lymphocyte percentage, D-dimer, and interleukin-6 (IL-6), were analyzed and compared between the two groups. Results: The median NLR was significantly higher in critical patients compared to non-critical patients (6.35 vs 4.00; p<0.001). Lymphopenia was more frequent in the critical group (p<0.001). Median D-dimer and IL-6 levels were markedly elevated among critical patients (797 ng/mL vs 140 ng/mL and 68.2 pg/mL vs 8.45 pg/mL, respectively; p<0.001). Conclusion: Elevated NLR, lymphopenia, and increased IL-6 and D-dimer levels are reliable predictors of COVID-19 severity and may assist in early risk stratification and clinical decision-making.
Keywords: COVID-19, Neutrophil-to-lymphocyte ratio, IL-6, D-dimer, Hematological markers, Disease severity
INTRODUCTION
Coronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has resulted in significant global morbidity and mortality. Clinical manifestations range from asymptomatic infection and mild respiratory illness to severe pneumonia, acute respiratory distress syndrome (ARDS), multiorgan dysfunction, and death. Early identification of patients at risk of progression to severe disease remains a major clinical challenge.
Severe COVID-19 is characterized by dysregulated immune responses, excessive cytokine release (cytokine storm), endothelial injury, and a hypercoagulable state. Hematological parameters obtained from routine blood investigations reflect these pathophysiological changes. Neutrophil-to-lymphocyte ratio (NLR) serves as a marker of systemic inflammation, while lymphopenia reflects immune exhaustion and impaired cellular immunity. Elevated interleukin-6 (IL-6) levels indicate cytokine-mediated inflammatory responses, and increased D-dimer levels signify activation of coagulation and fibrinolysis.
Several international studies have demonstrated the prognostic value of NLR, lymphocyte count, IL-6, and D-dimer in predicting COVID-19 severity and mortality. However, prospective data from Indian populations, particularly from resource-limited healthcare settings, remain limited. The present study was undertaken to evaluate the role of selected hematological and inflammatory markers as predictors of disease severity in hospitalized COVID-19 patients from South India.
MATERIALS AND METHODS
Study Design and Setting
This prospective observational study was conducted at Prathima Institute of Medical Sciences, Telangana, India, from December 2020 to October 2022.
Study Population
A total of 100 patients with laboratory-confirmed COVID-19 (RT-PCR positive) were included. Patients with hematological malignancies, known hematological disorders, or pregnancy were excluded from the study.
Severity Classification
Patients were categorized based on World Health Organization (WHO) COVID-19 severity guidelines.
Critical group: Patients requiring intensive care unit (ICU) admission, ventilatory support, or having severe hypoxia (SpO₂ <90% on room air).
Non-critical group: Patients not fulfilling the above criteria.
Laboratory Parameters
Blood samples collected at admission were analyzed for complete blood counts, neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), D-dimer, interleukin-6 (IL-6), ferritin, and lactate dehydrogenase (LDH) using standardized automated analyzers.
Ethical Approval
The study was approved by the Institutional Ethics Committee (IEC/PIMS/PG/2020/001). Written informed consent was obtained from all participants.
Statistical Analysis
Continuous variables were expressed as median and interquartile range (IQR). Comparisons between groups were performed using the Mann–Whitney U test. A p value <0.05 was considered statistically significant.
RESULTS
The study population had a median age of 50 years, with a male predominance (74%). Critical patients demonstrated significantly higher median NLR values and lower lymphocyte percentages compared to non-critical patients. Lymphopenia was observed in 72% of the study population and was significantly more frequent in the critical group (p<0.001).
D-dimer and IL-6 levels were markedly elevated among critical patients, indicating an association with severe disease (p<0.001). Other hematological and biochemical parameters, including hemoglobin, PLR, ferritin, and LDH, did not show a statistically significant correlation with disease severity.
|
Parameter |
Non-Critical |
Critical |
p-value |
|---|---|---|---|
|
NLR |
4.00 [2.67–5.40] |
6.35 [4.00–8.62] |
<0.001 |
|
Lymphocytes (%) |
20.0 [15.0–25.8] |
13.0 [10.0–19.2] |
<0.001 |
|
D-dimer (ng/mL) |
140 [114–200] |
797 [628–1160] |
<0.001 |
|
IL-6 (pg/mL) |
8.45 [4.53–11.1] |
68.2 [43.0–92.0] |
<0.001 |
Table 1: Hematological markers in Critical vs Non critical COVID-1 patients
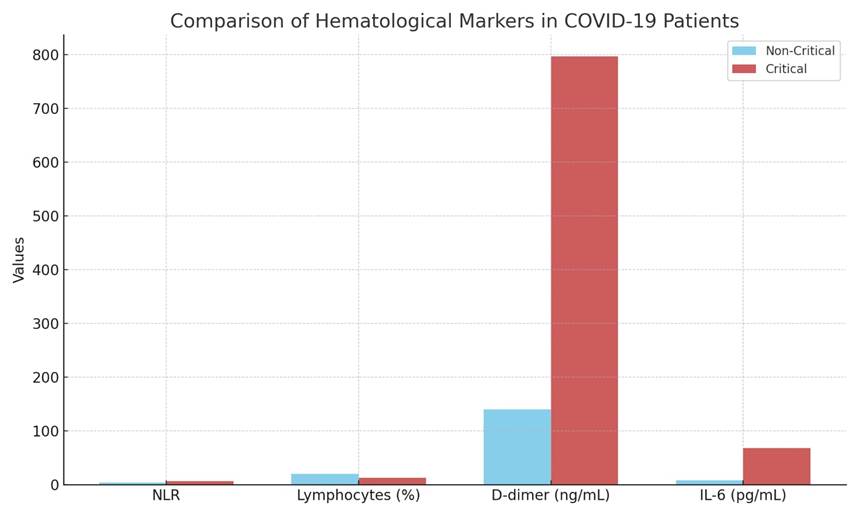
DISCUSSION
The present prospective study demonstrates that simple hematological and inflammatory markers are strongly associated with COVID-19 severity. Elevated NLR reflects neutrophil-driven systemic inflammation coupled with lymphocyte depletion due to immune exhaustion and apoptosis. Lymphopenia has been consistently reported as a hallmark of severe COVID-19 and is associated with poor outcomes.
Interleukin-6 plays a central role in cytokine-mediated inflammatory responses and is a key driver of cytokine storm. Elevated IL-6 levels observed in critically ill patients in this study support its role as a severity marker. Similarly, increased D-dimer levels reflect activation of coagulation pathways and endothelial dysfunction, both of which contribute to thrombotic complications and disease progression.
Our findings are consistent with earlier studies by Liao et al., Terpos et al., and other international and regional investigations that highlighted the prognostic utility of NLR, IL-6, lymphopenia, and D-dimer. The use of these inexpensive and widely available laboratory parameters is particularly valuable in resource-constrained healthcare systems [1-5].
The limitations of this study include its single-center design, modest sample size, and inclusion of patients across multiple pandemic waves, which may have influenced disease characteristics and management strategies.
CONCLUSION
Simple hematological and inflammatory markers such as neutrophil-to-lymphocyte ratio, lymphocyte percentage, interleukin-6, and D-dimer are reliable predictors of COVID-19 severity. Incorporation of these parameters at the time of hospital admission may aid early triaging, risk stratification, and optimal utilization of healthcare resources.
DISCLOSURE
Acknowledgments: The authors acknowledge the Department of Pathology, Prathima Institute of Medical Sciences, for their support in conducting this study.
Funding: No external funding was received for this study.
Competing Interests: The authors declare no conflicts of interest.
References
1. Liao D, Zhou F, Luo L, Xu M, Wang H, Xia J, et al. Haematological characteristics and risk factors in the classification and prognosis evaluation of COVID-19: a retrospective cohort study. The Lancet Haematology. 2020; 7 (9). Available from: https://doi.org/10.1016/s2352-3026(20)30217-9
2. Terpos E, Ntanasis-Stathopoulos I, Elalamy I, Kastritis E, Sergentanis TN, Politou M, et al.. Hematological findings and complications of <scp>COVID</scp>‐19. American Journal of Hematology. 2020; 95 (7). Available from: https://doi.org/10.1002/ajh.25829
3. Toori KU, Qureshi MA, Chaudhry A. Lymphopenia: A useful predictor of COVID-19 disease severity and mortality. Pakistan Journal of Medical Sciences. 2021; 37 (7). Available from: https://doi.org/10.12669/pjms.37.7.4085
4. Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. The Lancet. 2020; 395 (10223). Available from: https://doi.org/10.1016/s0140-6736(20)30183-5
5. World Health Organization. Clinical management of COVID-19. 2020.
Copyright
©2026 (Varun) et al. This is an open-access journal, and articles are distributed under the terms of the Creative Commons Attribution License CC-BY 4.0. (https://creativecommons.org/licenses/by/4.0/) which permits unrestricted use, distribution, and reproduction in any medium, provided the original authors and source are credited.
Cite this article
Varun K, Parveen SR, Anjum A, Naidu AT, Padmaja B. Hematological Markers as Predictors of COVID-19 Severity: A Prospective Study
from South India. Perspectives in Medical Research 2026; 14(1):37-39 DOI: 10.47799/pimr.1401.25.69